- Represents 6-8% of back and leg pain cases each year
Pyriformis Syndrome is a frequently unrecognized source of acute, subacute or chronic low back and leg pain. Acute pain is defined as pain of less than 12 weeks duration. Subacute pain is defined as pain of greater than 12 weeks duration but less than 6 months duration. Chronic pain is defined as pain of greater than 6 months duration. - Where is the Pyriformis Muscle?
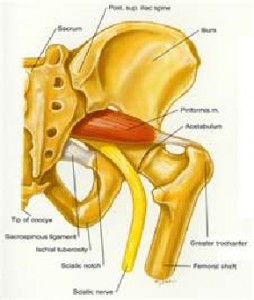
The pyriformis muscle is a deep muscle that lies under the gluteus maximus. Its origin is from the anterior sacrum and travels through the greater sciatic notch to insert on the greater trochanter of the femur. As such, the muscle lies directly over the sciatic nerve. Pain occurs as a consequence of spasm in the muscle. Because of the proximity of the pyriformis muscle to the sciatic nerve, that spasm causes compression of the sciatic nerve and consequent burning, electric or lancinating pain which will extend from the buttock down the posterior aspect of the thigh and calf to the foot. - What are the Causes of a Pyriformis Syndrome and How is it Diagnosed?
A Pyriformis Syndrome can be caused by running, cycling, weight lifting or direct trauma as from a fall and landing on the buttock. When persistent it is easily and frequently misdiagnosed as a lumbar radiculopathy, especially if MRI of the lumbar spine demonstrates a disc bulge or small herniation at the L4-5 or L5-S1 level. Physical examination is helpful in distinguishing between the two. In a Pyriformis Syndrome, pressure over the sciatic notch will reproduce the pattern of pain and the straight leg exam is frequently negative. Conversely, in a lumbar radiculopathy the straight leg raise test is positive early and there is usually no pain on pressure over the sciatic notch. In complicated cases, further diagnostic testing can help differentiate between the two. In a Pyriformis Syndrome, a lumbar epidural steroid injection will produce little to no benefit; while in a lumbar radiculopathy, the epidural injection will frequently produce a 50% or greater reduction in pain. Conversely, injection of a local anesthetic into the pyriformis under CT guidance will frequently produce a temporary but complete elimination of pain from a Pyriformis Syndrome and will have no effect with a lumbar radiculopathy. It is important to note that the two can coexist. It is therefore important to consider a Pyriformis Syndrome in those cases where leg pain persists after surgery for a lumbar radiculopathy. - What is the Treatment for a Pyriformis Syndrome?
Pyriformis Syndrome is diagnosed by reproducing the pattern of pain by applying pressure over the sciatic notch. Confirmation of the diagnosis is achieved by injecting the pyriformis with a local anesthetic under CT guidance. A 50% or greater reduction in pain for at least 1-2 hours is considered confirmatory. In rare cases, the local anesthetic injection will be curative but in the majority of cases the pain will recur once the anesthetic has worn off. The treatment of choice is then injection of Botox under CT guidance which will typically produce pain relief of 3 months duration or greater. The duration of pain relief may be extended if the Botox injection is coupled with physical therapy specifically directed at the pyriformis.
2. Psoas Syndrome
- Frequently Unrecognized Source of Back Pain
The Psoas Syndrome is a frequently unrecognized source of acute, subacute or chronic low back pain. Acute back pain is defined as pain of less than 12 weeks duration. Subacute back pain is defined as pain of greater than 12 weeks duration and less than 6 months duration. Chronic low back pain is defined as pain of greater than 6 months duration. - Where is the Psoas Muscle?
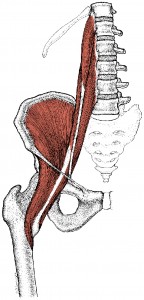
The iliopsoas muscle lies deep in the abdominal cavity and runs from its origin along the lateral surface of the lumbar spine to its insertion at the greater trochanter of the femur. Pain occurs as a consequence of spasm in the muscle and is usually perceived as low back pain with or without referral to the hips. - What are the Causes of a Psoas Syndrome?
A Psoas Syndrome can be caused by running (especially uphill); sitting, kneeling or crouching for extended periods of time; kicking; skating; lifting; or direct trauma to the abdomen as from a lap restraint in a motor vehicle accident. When persistent it is easily and frequently misdiagnosed as a lumbar strain, pain from lumbar disc pathology or pain from degeneration of the facet joints in the lumbar spine. Failure to recognize a psoas syndrome can consequently lead to failed efforts at physical therapy mistakenly directed toward the lumbar musculature. Lack of recognition may also be responsible for ineffective interventional techniques such as epidural injections, facet joint blocks and rhizotomies where asymptomatic degenerative changes identified on MRI or CT are assumed to be the source of pain. In extreme cases, this may even lead to unnecessary and ineffective spine surgery. - How is a Psoas Syndrome Diagnosed and What is the Treatment?
Psoas Syndrome is diagnosed by physical examination. Pressure in the inguinal region over the psoas reveals tightness and reproduces the patient’s back pain. The clinical diagnosis is then confirmed by injection of local anesthetic into the psoas muscle under CT guidance. Pain relief is usually immediate and the anesthetic typically produces at least a 50% reduction in pain. In some cases the pain relief is permanent in which case the injection is therapeutic as well as diagnostic. In most cases, the pain will recur within hours to days of the injection, in which case the treatment of choice is an injection of Botox into the psoas under CT guidance. Botox will typically produce pain relief of at least 3 months duration. The duration of relief may be extended if the Botox injection is coupled with therapy specifically directed toward the iliopsoas.
If you believe you are suffering from one of these back pain syndromes, schedule an appointment for evaluation through the Northstar Pain Care Maple Grove office.








I’m really loving the theme/design of your site. Do you ever run into any internet browser compatibility problems? A few of my blog audience have complained about my website not operating correctly in Explorer but looks great in Safari. Do you have any solutions to help fix this problem?
I love what you guys are usually up too. This sort of clever work and reporting! Keep up the amazing works guys I’ve you guys to my own blogroll.